Scleral Lens Fit For Severe Exposure Keratopathy Secondary to Bilateral Eyelid Colobomas
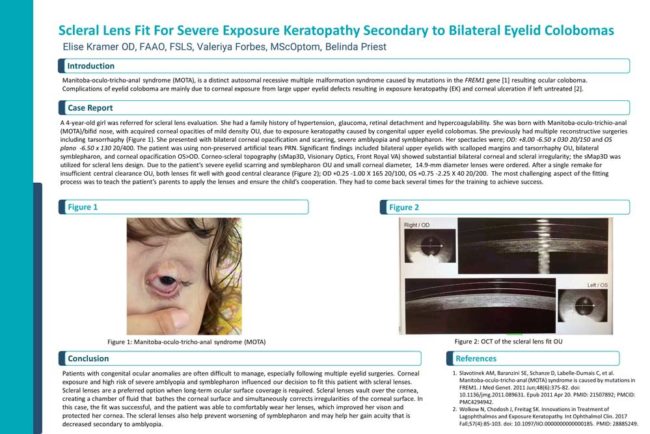
Manitoba-oculo-tricho-anal syndrome (MOTA), is a distinct autosomal recessive multiple malformation syndrome caused by mutations in the FREM1 gene [1] resulting ocular coloboma.